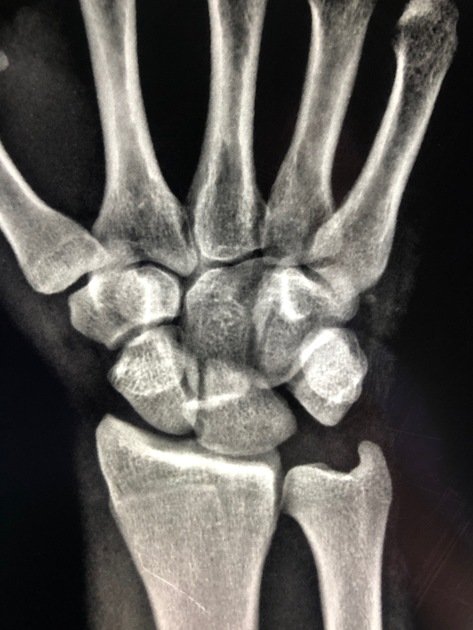
Overview & Classification Framework
Perilunate dislocations (PLDs) and perilunate fracture-dislocations (PLFDs) represent the most severe acute carpal injuries, sitting at the extreme end of the spectrum of carpal instability. They involve a catastrophic disruption of the carpal ligamentous architecture, in which the entire distal carpal row — along with the scaphoid, triquetrum, and hamate — is displaced dorsally relative to the lunate, which remains seated in the lunate fossa of the distal radius. In the most advanced stage (lunate dislocation), the lunate itself is pushed volarly out of the lunate fossa into the carpal tunnel. They are rare injuries, accounting for approximately 7–10% of all carpal fractures and dislocations, and occur predominantly in young males from high-energy trauma.
- Lesser arc vs greater arc injuries (Cooney): the trajectory of force through the carpus determines whether the disruption is purely ligamentous (`lesser arc`) or passes through bone (`greater arc`); the lesser arc is the zone immediately surrounding the lunate — ligaments only (scapholunate, lunotriquetral, capitolunate); a lesser arc injury = pure perilunate dislocation (no fractures); the greater arc is a wider zone that passes through the bones surrounding the lunate (scaphoid waist, capitate head, hamate body, triquetrum) — a greater arc injury = perilunate fracture-dislocation; the most common greater arc injury is the `trans-scaphoid perilunate fracture-dislocation` (the scaphoid waist fractures as the force passes through the radial side — the proximal pole remains with the lunate while the distal pole displaces with the rest of the carpus)
- Epidemiology: predominantly young adult males (peak age 20–40 years); high-energy mechanisms (road traffic accidents, falls from height, industrial crush injuries); associated with polytrauma; frequently missed at initial assessment (up to 25% delayed diagnosis); trans-scaphoid perilunate fracture-dislocation is the most common greater arc pattern (60% of all PLDs/PLFDs)
Mechanism & Mayfield Classification
The Mayfield classification (1980) describes the progressive perilunar instability sequence as a predictable four-stage failure of the carpal ligaments in a specific circumferential direction, beginning radially (at the scapholunate interval) and propagating in an ulnar direction around the lunate. Each stage represents a discrete increment of ligamentous failure.
| Mayfield Stage | Ligament Failure | Clinical Entity | Radiological Correlate |
|---|---|---|---|
| Stage I | Scapholunate ligament disruption (the scapholunate interosseous ligament — SLIL — ruptures; also the dorsal and volar radioscaphoid ligaments); the scaphoid rotates into flexion and the lunate extends — creating the dorsal intercalated segment instability (DISI) pattern; the scapholunate gap opens | Scapholunate dissociation (SLD) — the mildest form of perilunar instability; isolated SLD without further carpal progression | AP view: Terry Thomas sign (scapholunate gap >3 mm — `gap between front teeth`); cortical ring sign (the scaphoid appears foreshortened and round as it rotates into flexion); DISI on lateral view (lunate dorsiflexed — scapholunate angle >70°) |
| Stage II | The disruptive force propagates through the space of Poirier (the `weak zone` in the volar capitolunate ligaments — this is the most vulnerable point in the volar carpal ligamentous architecture); the capitate dislocates dorsally relative to the lunate; the capitolunate joint dislocates while the scapholunate joint remains disrupted | Perilunate dislocation — the capitate is dorsal to the lunate; the lunate remains in the lunate fossa | Lateral X-ray: the capitate is dorsal to the lunate — the normal colinear alignment of the radius-lunate-capitate is lost; the lunate appears as a `pie slice` or `D-shape` on the lateral view (tilted volarly into extension); AP view: overlapping carpal bones, loss of Gilula`s arcs |
| Stage III | The disruption continues ulnarly — the lunotriquetral interosseous ligament (LTIL) ruptures; the triquetrum dislocates dorsally from the lunate; the entire distal carpal row (scaphoid + capitate + hamate + triquetrum) is now displaced dorsally relative to the lunate; the lunate remains in the lunate fossa | Complete perilunate dislocation — the lunate is the only proximal carpal bone remaining in the lunate fossa; all others are displaced dorsally | The classic perilunate dislocation radiograph; AP view: complete disruption of all three Gilula arcs; lateral view: the lunate is in the lunate fossa but the capitate, scaphoid, and triquetrum are all dorsal to it; the lunate still faces the radius but is beginning to tilt |
| Stage IV | The lunate is completely levered out of the lunate fossa by the progressive dorsal force; the lunate rotates 90° or more volarly (the dorsal cortex becomes anterior) and dislocates anteriorly into the carpal tunnel; the capitate drops into the lunate fossa vacated by the lunate; the lunate is now anterior to the carpal tunnel, compressing the median nerve | True lunate dislocation (the most severe form — commonly confused with perilunate dislocation; the distinction is the position of the lunate: in perilunate dislocation the lunate is in situ; in lunate dislocation the lunate has been expelled anteriorly into the carpal tunnel) | Lateral X-ray: the `spilled teacup sign` — the lunate is volarly displaced and rotated (its concave surface points anteriorly rather than dorsally — as if the teacup has been tipped and spilled); the capitate drops into the empty lunate fossa; AP view: the lunate appears triangular (`pie slice`) and overlaps the distal radius; the capitate occupies the lunate fossa position |
Radiological Diagnosis — Gilula`s Arcs & Key Signs
- Gilula`s three carpal arcs (AP view): on a standard PA wrist radiograph in neutral position, three smooth continuous arcs should be identifiable; Arc I — the proximal convex surfaces of the scaphoid, lunate, and triquetrum (a smooth curve); Arc II — the distal concave surfaces of the scaphoid, lunate, and triquetrum (parallel to Arc I); Arc III — the proximal convex surfaces of the capitate and hamate; in a normal wrist, all three arcs are smooth, continuous, and parallel; ANY disruption, step-off, or discontinuity in these arcs indicates carpal instability or dislocation; in a perilunate dislocation, Arcs I, II, and III are all disrupted and the carpal bones overlap each other on the AP view creating a `crowded` appearance
- Key radiological signs summary: (1) AP view — loss of Gilula`s arcs; Terry Thomas sign (SL gap >3 mm); cortical ring sign (foreshortened scaphoid); triangular `pie-slice` lunate; overlapping carpal bones; (2) Lateral view — loss of the normal colinear radius-lunate-capitate alignment; DISI pattern (scapholunate angle >70°, capitolunate angle >30°); the capitate is dorsal to the lunate (perilunate) OR the lunate is volar to the capitate (lunate dislocation — `spilled teacup`); (3) AP + Lateral combined — the lateral view is the single most important view for diagnosis; most missed diagnoses are due to failure to examine the lateral view carefully
- The `spilled teacup sign` (lunate dislocation): on the lateral wrist X-ray, the lunate normally appears as a `C` shape opening posteriorly (the concave surface faces the capitate); in a true lunate dislocation, the lunate has rotated 90° volarly — the `C` now opens anteriorly, like a teacup that has been tipped forward and spilled its contents; this sign is pathognomonic of Stage IV lunate dislocation; the capitate falls into the empty lunate fossa on the AP view; the AP view alone can appear misleadingly unremarkable — the lateral view is essential
Clinical Assessment
- History: significant trauma (high-energy fall, road traffic accident, sports); immediate severe wrist pain and swelling; inability to use the hand; the patient may present with the hand already splinted after the injury
- Examination: the wrist is swollen, tender, and deformed (a dorsal prominence may be visible from the dorsally displaced carpus; in lunate dislocation, a volar prominence is palpable in the carpal tunnel region); range of motion is severely restricted; ALWAYS assess median nerve function — acute carpal tunnel syndrome is present in up to 25% of perilunate dislocations and up to 45% of lunate dislocations; assessment: two-point discrimination index finger and thumb (median nerve sensory); thenar muscle power (abductor pollicis brevis — APB — median nerve motor); symptoms: paraesthesia in the thumb, index, middle, and radial ring fingers; thenar atrophy (if presentation is delayed)
- Vascular assessment: the radial and ulnar pulses must be documented before and after any reduction attempt; vascular injury is uncommon but reported; the radial artery may be injured by the displaced scaphoid in trans-scaphoid variants; Doppler assessment if pulses are absent or diminished
Investigations
- Plain radiographs: AP, lateral, and oblique views of the wrist are the mandatory initial investigation; the lateral view is the most diagnostically important — examine carefully for the radius-lunate-capitate alignment; the AP view demonstrates Gilula`s arc disruption; the diagnosis is frequently missed because: (1) the AP view may appear confusingly `crowded` rather than obviously abnormal; (2) the lateral view is not examined carefully; (3) the treating clinician is not familiar with the normal carpal relationships; a systematic approach to every wrist X-ray (check Gilula`s arcs on AP; check R-L-C alignment on lateral) prevents missed diagnoses
- CT scan: mandatory for all confirmed or suspected perilunate injuries; provides: (1) definitive characterisation of the injury pattern (lesser vs greater arc; exact bones fractured); (2) the scaphoid fracture pattern and displacement in trans-scaphoid variants (guides fixation planning); (3) identification of associated fractures (capitate, triquetrum, hamate); (4) 3D reconstruction for complex surgical planning; CT should be obtained AFTER initial closed reduction (if performed) to reassess the post-reduction carpal anatomy
- MRI: used selectively; most valuable for: (1) assessing the integrity of the scapholunate and lunotriquetral interosseous ligaments (critical for surgical repair planning); (2) evaluating associated chondral injuries; (3) assessing median nerve compression within the carpal tunnel; (4) detecting associated triangular fibrocartilage complex (TFCC) injuries; in clinical practice, MRI is often performed post-operatively to assess ligament healing rather than pre-operatively, where CT is more actionable for surgical planning
- Nerve conduction studies (NCS): not required acutely; indicated post-operatively if median nerve symptoms persist to assess recovery and guide further management
Management — Emergency & Definitive
| Phase | Intervention | Detail |
|---|---|---|
| Acute (Emergency) | Closed reduction under sedation or GA | Urgent closed reduction is performed as soon as the patient is medically appropriate — typically within hours of presentation; the aim is to reduce the acute carpal tunnel pressure and decompress the median nerve; technique (the Tavernier manoeuvre for perilunate/lunate dislocation): (1) finger trap traction applied for 5–10 minutes to distract the carpus; (2) the surgeon applies longitudinal traction with one hand while the thumb of the other applies direct dorsal pressure on the lunate (for lunate dislocation — pressing the lunate back into the lunate fossa from the volar prominence); (3) simultaneous wrist extension followed by progressive wrist flexion to relocate the lunate into the fossa; (4) for perilunate dislocation — the wrist is extended under traction then progressively flexed; a `clunk` confirms reduction; post-reduction splint in slight wrist flexion; post-reduction AP + lateral and CT to assess quality of reduction; closed reduction does NOT achieve ligamentous healing and is NOT definitive treatment — it is an emergency temporising measure |
| Definitive (Days 1–7) | Open reduction + ligament repair + K-wire fixation | Definitive surgical treatment should be performed within 5–7 days of injury (before soft tissue swelling and early fibrosis make dissection more difficult and reduction harder to achieve); the procedure is typically performed through BOTH dorsal AND volar approaches: (1) DORSAL approach first — between the 3rd and 4th extensor compartments (between EPL and EDC); the dorsal capsule is opened longitudinally (the `ligament-sparing capsulotomy` — the dorsal intercarpal and dorsal radiocarpal ligaments are preserved or incised at their insertion to allow repair); the carpus is reduced under direct visualisation; K-wires are placed to provisionally hold the reduction (scaphocapitate K-wire; scapholunate K-wire; lunotriquetral K-wire); the scaphoid fracture (in trans-scaphoid variants) is fixed with a headless compression screw (Herbert or Acutrak) under fluoroscopic guidance; the dorsal SLIL is repaired with suture anchors; (2) VOLAR approach — the carpal tunnel is released (median nerve decompression — mandatory in all cases); the volar SLIL, volar lunotriquetral ligament, and space of Poirier are repaired with suture anchors or direct suture; the radio-scapho-capitate (RSC) ligament is repaired if torn; the wrist is immobilised in a cast after surgery |
| Delayed presentation (>3 weeks) | Open reduction ± proximal row carpectomy or limited wrist arthrodesis | Open reduction is significantly more difficult after 3 weeks (fibrous tissue forms in the joint spaces, preventing reduction without extensive release); outcomes of late open reduction are substantially worse; if open reduction is achieved → K-wire fixation + ligament repair as above; if anatomical reduction is not possible → salvage procedures: proximal row carpectomy (PRC — excision of the scaphoid, lunate, and triquetrum, allowing the capitate to articulate with the radius; provides reasonable function), or four-corner arthrodesis (scaphoid excision + lunate-capitate-hamate-triquetral fusion); total wrist arthrodesis for end-stage post-traumatic arthritis |
| Post-operative | Immobilisation then rehabilitation | Above-elbow cast for 6 weeks (protects the K-wires and the ligament repairs); below-elbow cast or removable splint for a further 6 weeks; K-wires removed under local anaesthetic at 8–10 weeks; hand therapy — progressive wrist ROM exercises, grip strengthening, proprioception training; return to light work at 3–4 months; return to manual or heavy work at 6–12 months; formal grip strength and ROM assessment at 6 months and 12 months |
Trans-Scaphoid Perilunate Fracture-Dislocation
- The most common greater arc injury (60% of all PLDs): in a trans-scaphoid PLFD, the force vector passes through the scaphoid waist rather than through the scapholunate ligament; the scaphoid waist fractures; the proximal scaphoid pole remains attached to the lunate via the intact proximal SLIL and moves with the lunate (remains in the lunate fossa); the distal scaphoid fragment displaces dorsally with the rest of the carpus (capitate, hamate, triquetrum); radiologically: the scaphoid fracture is visible on the AP view; the lunate remains in situ but the distal carpus is dorsal; the `de Quervain`s fracture-dislocation` is the same injury named eponymically
- Surgical management of the scaphoid fracture: the scaphoid fracture is fixed with a headless compression screw (Herbert/Acutrak) placed along the central axis of the scaphoid under fluoroscopic guidance — this is performed through the dorsal approach as part of the definitive combined procedure; the proximal pole fragment (still attached to the lunate) serves as the `anchor` and the distal pole is reduced to it; the screw provides compression across the fracture; bone grafting is occasionally required if there is a significant fracture gap after reduction; AVN of the proximal scaphoid pole is a risk (the retrograde blood supply is disrupted by the dislocation and possibly by the trauma) but is less common than in isolated proximal pole scaphoid fractures because the lunate`s retained vascular supply partially protects the proximal pole
Complications & Outcomes
- Carpal instability (DISI pattern): residual scapholunate dissociation after inadequate ligament repair; the scaphoid rotates into flexion and the lunate extends; presents as `clunking` wrist, pain with wrist extension and radial deviation, and grip weakness; managed with ligament reconstruction (RASL procedure — reduction and association of the scaphoid and lunate with a screw), tendon graft reconstruction (three-ligament tenodesis), or salvage (four-corner fusion or PRC); the degree of residual carpal instability directly predicts the rate of post-traumatic arthritis
- Post-traumatic wrist arthritis (SLAC wrist — scapholunate advanced collapse): the most important long-term complication; occurs in a predictable pattern identical to SLAC wrist from untreated SL dissociation: Stage I (radial styloid-distal scaphoid arthritis) → Stage II (entire radioscaphoid arthritis) → Stage III (capitolunate arthritis); the rate and severity of SLAC wrist progression correlates with the quality of carpal reduction and ligament repair; management of established SLAC: four-corner arthrodesis (scaphoid excision + LC-HC-TC fusion) for Stages II–III; total wrist arthrodesis for end-stage
- Median nerve injury: acute carpal tunnel syndrome is the most common neurological complication (25–45%); the median nerve is compressed by the volarly displaced lunate; usually a neuropraxia that resolves after reduction and carpal tunnel release; persistent median nerve symptoms at 3 months → NCS/EMG assessment; chronic median nerve injury from delayed diagnosis requires carpal tunnel release + neurolysis; permanent thenar atrophy may result from prolonged compression
- Avascular necrosis of the lunate: uncommon but reported; the lunate`s blood supply enters through dorsal and volar ligamentous attachments — if all attachments are torn, AVN can develop; presents as progressive lunate sclerosis and collapse on serial X-rays; MRI confirms AVN; management — core decompression (early), vascularised bone graft, or salvage arthroplasty/fusion depending on stage
- Outcomes: even with prompt anatomical reduction and meticulous surgical repair, long-term wrist function is frequently impaired; mean grip strength at 5 years is approximately 70–80% of the contralateral side; mean ROM is approximately 50–60% of the contralateral side; pain scores improve significantly but chronic aching with heavy use is common; return to heavy manual work is often limited; outcomes are substantially worse with delayed diagnosis (>3 weeks) or inadequate initial reduction
Exam Pearls
- Mayfield stages: I (SL ligament — SLD/DISI); II (space of Poirier — perilunate dislocation, capitate dorsal); III (LT ligament — complete perilunate, all carpus dorsal); IV (lunate expulsion into carpal tunnel — lunate dislocation)
- Lesser arc (ligamentous only) vs greater arc (through bone — trans-scaphoid most common, 60%): the scaphoid fractures through its waist; proximal pole stays with lunate; distal pole displaces dorsally with the carpus
- Gilula`s three arcs: smooth continuous arcs on PA wrist X-ray; ANY disruption = carpal instability; Arc I = proximal convex surfaces of proximal row; Arc II = distal concave surfaces of proximal row; Arc III = proximal convex surfaces of capitate and hamate
- Spilled teacup sign (Stage IV lunate dislocation): the lunate rotates 90° volarly; its concave articular surface faces anteriorly (the `C` opens forward) rather than posteriorly; the capitate drops into the empty lunate fossa; the lateral X-ray is pathognomonic
- Median nerve compression: present in 25–45%; acute carpal tunnel syndrome; thenar paraesthesia and weakness (APB); volar carpal tunnel release is MANDATORY at the time of definitive surgery in ALL cases — even in the absence of pre-operative symptoms
- Surgical approach: DORSAL (reduction + K-wires + screw for scaphoid + dorsal SLIL repair) + VOLAR (carpal tunnel release + volar SLIL/LTIL repair + space of Poirier repair); both approaches required in virtually all cases
- Missed diagnosis (up to 25%): the most important preventable error; check Gilula`s arcs on EVERY wrist X-ray; examine the lateral view systematically (R-L-C colinear alignment); the AP view can appear `crowded` but non-specifically so — the lateral view is diagnostic; CT for all wrist injuries with mechanism suggesting high energy
- Delayed presentation (>3 weeks): outcomes significantly worse; open reduction increasingly difficult (fibrous ankylosis); salvage procedures (PRC, four-corner fusion) may be required at the time of first surgery; the urgency of diagnosis and treatment cannot be overemphasised