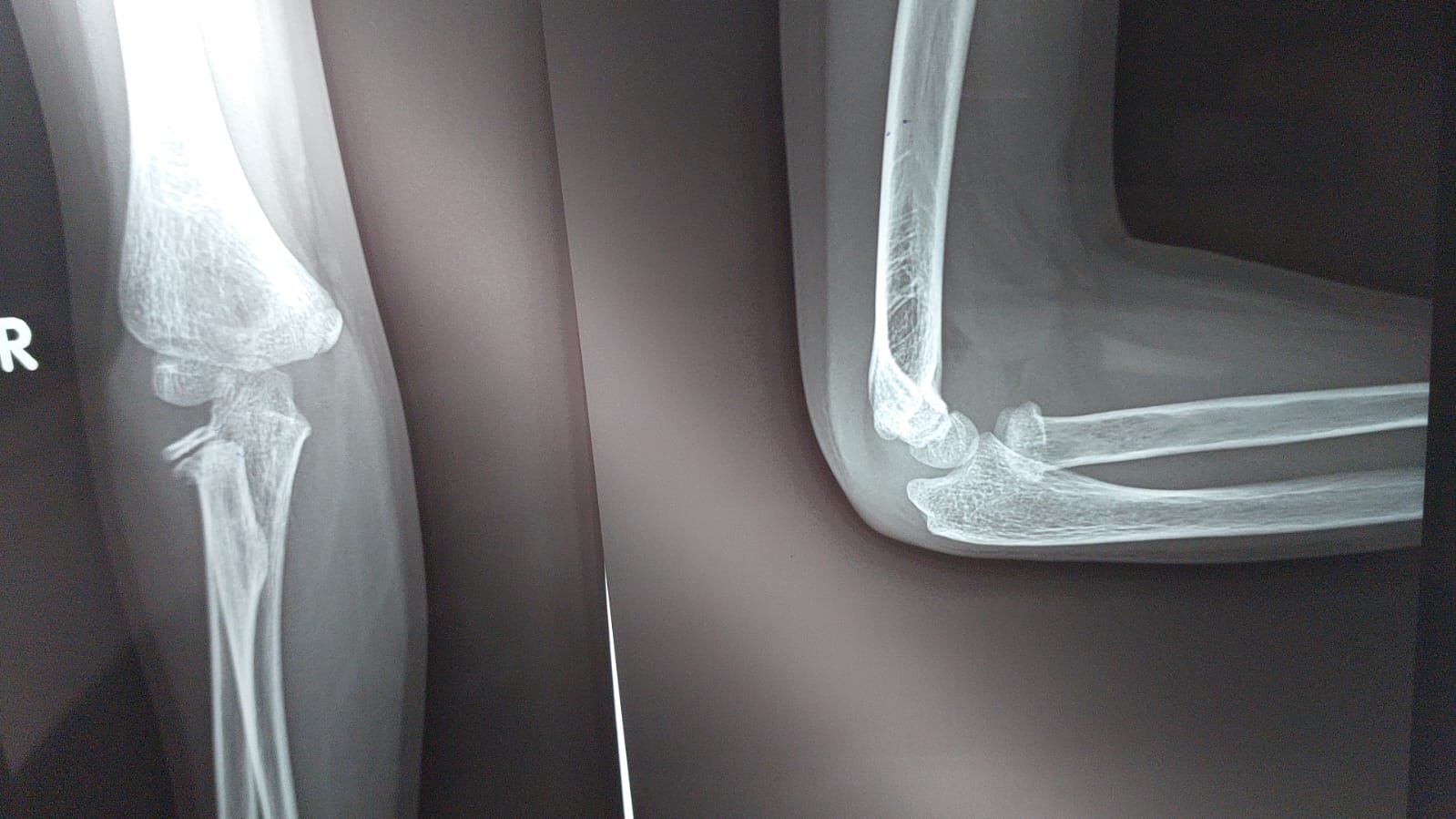
Overview — Radial Head Fractures
Radial head fractures are the most common fractures about the elbow in adults, accounting for approximately 33% of all elbow fractures. They occur most commonly from a fall onto an outstretched hand (FOOSH), during which axial compression transmits force from the wrist through the forearm to the radiocapitellar joint, fracturing the radial head as it impacts the capitellum. The Mason classification (1954), modified by Johnston (1962), Broberg and Morrey (1987), and Hotchkiss (1997), is the universal system for describing radial head fracture morphology and guides management — from conservative treatment for simple undisplaced fractures to arthroplasty for severely comminuted fractures.
- Anatomy: the radial head is the proximal articular end of the radius; it articulates with the capitellum of the distal humerus (radiohumeral joint) and with the radial notch of the ulna (proximal radioulnar joint); the radial head is a secondary stabiliser of the elbow against valgus stress (the primary valgus stabiliser is the anterior bundle of the MCL) and against axial loading through the forearm (the primary axial load transmitter is the interosseous membrane, but the radial head bears ~60% of the forearm axial load in the extended position); the blood supply to the radial head is limited — the `safe zone` for fixation hardware is the posterolateral 90° arc of the radial head (this arc does NOT articulate with the ulna in any forearm position and can therefore bear screws or plates without causing mechanical impingement)
- The `Essex-Lopresti` injury: a specific high-energy injury where the radial head is severely fractured AND the interosseous membrane is torn AND the DRUJ is disrupted; the entire longitudinal stability of the forearm is lost; the radius migrates proximally relative to the ulna; radial head excision alone (without replacement) in the Essex-Lopresti pattern catastrophically worsens the proximal radial migration; a metallic radial head arthroplasty is mandatory to restore the forearm length; always assess the DRUJ and the interosseous membrane in all radial head fractures before deciding on treatment
Mason Classification (Modified Hotchkiss)
| Mason Type | Fracture Description | Displacement | Forearm Rotation Block | Management |
|---|---|---|---|---|
| Type I — Undisplaced | A non-displaced or minimally displaced fracture of the radial head or neck; the fracture may be partial articular (marginal fragment) or a fissure fracture; the articular surface is intact or nearly so; displacement is <2 mm | <2 mm displacement; no significant articular step-off | NO mechanical block to forearm rotation — the undisplaced fragment does not interfere with pronation/supination; if forearm rotation is painful but free of mechanical block, the injury is a Type I | NON-OPERATIVE — aspiration of the elbow haemarthrosis (under LA) + sling for comfort for 1–2 weeks → early mobilisation (within 1 week); the haemarthrosis is the primary source of pain and stiffness; aspiration provides immediate pain relief and allows earlier motion; excellent functional outcomes with early mobilisation; do NOT immobilise for more than 2 weeks (joint stiffness risk) |
| Type II — Partial articular, displaced | A partial articular fracture involving part of the radial head (marginal fracture — one sector of the radial head is fractured); the fragment is displaced >2 mm; the fracture is fixable with standard fragment-specific techniques (the fragment is large enough to accept a screw); impaction of articular cartilage ± mechanical block to forearm rotation may be present | >2 mm displacement; articular step-off; the fragment may be tilted, displaced, or impacted | MAY have a MECHANICAL BLOCK to forearm rotation from the displaced fragment impinging on the proximal ulna or the capitellum; clinical test: `block test` — after aspiration and LA instillation, active or passive forearm rotation is assessed; if smooth full rotation is possible → no block → conservative management may be appropriate; if there is a block to rotation → ORIF or excision of the fragment | ORIF if: (1) mechanical block to forearm rotation; (2) displacement >2 mm (3 mm in some systems); (3) fragment >25–30% of the radial head (a fragment this size significantly affects joint mechanics and bears load); technique: Herbert screws or mini-fragment screws placed in the `safe zone` (posterolateral 90° arc — the non-articulating zone); elbow is approached via the Kocher (anconeus-ECU) or Kaplan (EDC-ECRB) approach; non-operative for undisplaced or asymptomatic Type II with no block (selected cases) |
| Type III — Comminuted, non-reconstructable | A COMMINUTED fracture of the entire radial head with multiple fragments; the fracture is NOT amenable to fixation (too many fragments, all <3 mm, no adequate surface for screw purchase); the radial head is essentially shattered; the fracture cannot be reconstructed by ORIF — the individual fragments are too small and comminuted for individual fixation | Extensive comminution; no single fixable fragment; the radial head is in multiple pieces | Mechanical block is invariably present from the comminution and displaced fragments; the radial head has lost its structural integrity; simple excision will create a mechanical block-free forearm but creates instability (particularly in the Essex-Lopresti pattern or with associated MCL injury); replacement with a metallic radial head prosthesis is preferred | METALLIC RADIAL HEAD ARTHROPLASTY — the radial head prosthesis restores forearm length, provides valgus stability, and prevents proximal radial migration; do NOT perform radial head EXCISION WITHOUT replacement in the terrible triad or Essex-Lopresti patterns (catastrophic instability will result); the prosthesis is placed in the `safe zone` (posterolateral); assess the DRUJ and MCL intraoperatively after arthroplasty |
| Type IV — With elbow dislocation (Johnston addition) | ANY Mason Type (I, II, or III) radial head fracture associated with an ELBOW DISLOCATION; the Johnston modification (1962) added this category to acknowledge that the combination of radial head fracture + elbow dislocation creates a distinct and more complex injury pattern; the combination is equivalent to the `terrible triad` if a coronoid fracture is also present | Variable displacement depending on underlying Mason Type; the elbow dislocation adds ligamentous and soft tissue injury to the bony fracture | The elbow dislocation has torn the lateral collateral ligament complex (and often the MCL) in addition to fracturing the radial head; even a Mason Type I fracture with an elbow dislocation requires careful reassessment of elbow stability after reduction; the terrible triad (posterior dislocation + radial head fracture + coronoid fracture) is a specific and serious form of Type IV injury | Reduce the elbow dislocation FIRST (closed reduction); reassess the radial head fracture and elbow stability after reduction; manage the radial head fracture according to its Mason type (I → conservative if stable; II → ORIF; III → arthroplasty); repair the LUCL and coronoid as part of the terrible triad protocol (see Article 150) |
Radial Head Arthroplasty — Indications & Considerations
- When to replace vs excise: the radial head should NEVER be excised without replacement in the following scenarios: (1) Essex-Lopresti injury (interosseous membrane tear + DRUJ disruption — the radial head is the only remaining axial forearm stabiliser after the IOM is torn; excision causes proximal radial migration and DRUJ arthritis); (2) terrible triad (posterior dislocation + radial head fracture + coronoid fracture — in an MCL-deficient elbow, the radial head provides critical valgus stability; excision creates catastrophic valgus instability); (3) valgus-varus instability from MCL injury at the time of the fracture; (4) any Mason III fracture with associated ligamentous instability; simple radial head excision without replacement may be appropriate ONLY for isolated Mason III fractures with no associated instability, in patients willing to accept the mild restriction of forearm rotation and the minor loss of grip strength
- Oversizing of radial head prosthesis (`overstuffing`): one of the most common technical errors in radial head arthroplasty; an oversized prosthesis distracts the radiocapitellar joint → increased capitellar wear → early capitellar OA → pain and stiffness; the radial head prosthesis should restore the native radial head height (measured from the radial neck to the articular surface on the intact side); check under fluoroscopy that the `lateral ulnohumeral joint space` is symmetric after prosthesis implantation (an asymmetric wider space indicates overstuffing)
Exam Pearls
- Mason classification: I (undisplaced <2 mm, no block — non-op, aspirate haematoma, early mobilisation); II (partial articular displaced >2 mm, fixable — ORIF if block or large fragment); III (comminuted, non-fixable — metallic radial head arthroplasty); IV (Johnston addition — any type with elbow dislocation)
- Safe zone for fixation hardware: posterolateral 90° arc of the radial head; does NOT articulate with the ulna in any forearm rotation position; place screws/plates here to avoid impingement on forearm rotation
- Essex-Lopresti injury: radial head fracture + interosseous membrane tear + DRUJ disruption; proximal radial migration; NEVER excise without replacement; metallic arthroplasty is mandatory; assess DRUJ and wrist in ALL radial head fractures
- Block test: after aspiration + LA, assess forearm rotation; if smooth rotation → no mechanical block → Type I/II without block → conservative management possible; if blocked → ORIF or arthroplasty
- Haemarthrosis aspiration: performed for all radial head fractures presenting acutely with a painful restricted elbow; a posterior lateral approach (posterolateral soft-spot approach — at the centre of the triangle formed by the radial head, lateral epicondyle, and olecranon tip); provides immediate pain relief and allows assessment of mechanical block; instil LA (1% lignocaine) after aspiration
- Radial head prosthesis overstuffing: distraction of the lateral ulnohumeral joint; early capitellar wear and pain; check under fluoroscopy after implantation that the lateral joint space is symmetric
- Radial head as secondary valgus stabiliser: the primary valgus stabiliser = anterior bundle of the MCL; the radial head is the secondary stabiliser; in an MCL-deficient elbow (tear or inadequate repair), the radial head MUST be preserved or replaced to prevent valgus instability; this is the biomechanical rationale for arthroplasty rather than excision in the terrible triad