Overview & Definition
A mega-prosthesis (modular tumour endoprosthesis) is a large segmental implant designed to replace a major portion of a long bone — including its articular surface — following en-bloc resection of bone tumours, extensive periprosthetic fractures with massive bone loss, or failed arthroplasty with severe bone deficiency. Unlike standard joint replacement prostheses, mega-prostheses replace not just the joint surface but the entire metaphysis and a variable length of the diaphysis. They are modular, allowing the surgeon to assemble the appropriate length and diameter of implant intraoperatively to match the resected bone segment. The indications have expanded from purely oncological to include complex non-oncological reconstruction, but the principles — adequate stem fixation, soft tissue reconstruction, and careful patient selection — remain constant.
- Oncological indications: primary malignant bone tumours requiring wide resection — osteosarcoma (most common; typically around the knee — distal femur 40%, proximal tibia 20%); Ewing sarcoma; chondrosarcoma; malignant giant cell tumour; metastatic bone disease with impending or actual pathological fracture not amenable to internal fixation (predicted survival >3 months — the Mirels scoring system guides prophylactic fixation); reconstruction after tumour resection at the proximal femur, proximal humerus, distal femur, proximal tibia, and pelvis are the most common mega-prosthetic sites
- Non-oncological indications: complex periprosthetic fractures with massive bone loss where standard ORIF or conventional revision arthroplasty is not feasible; failed revision arthroplasty with severe bone stock deficiency (AORI Type III for TKA; Paprosky Type IIIB for THA); distal femur fractures in elderly osteoporotic patients with highly comminuted bone not suitable for fixation (mega-prosthesis as primary treatment — immediate weight-bearing, shorter rehabilitation); chronic distal femur non-union in elderly patients
Design & Available Systems
- Modular design: modern mega-prostheses are modular — they consist of a joint surface component (femoral condylar component, tibial plateau, femoral head), metaphyseal body segments (available in different lengths — assembled to match the resected bone length), diaphyseal stem (intramedullary — available in different lengths and diameters; cemented or cementless press-fit), and interconnecting modular couplers; modularity allows intraoperative adjustment to the precise resection length — this contrasts with older custom-made (monoblock) prostheses that required pre-operative manufacturing based on imaging predictions of resection length and carried the risk of intraoperative mismatch
- The hydroxyapatite (HA) collar: a porous hydroxyapatite-coated collar at the bone-prosthesis junction (the point where the implant meets the cut end of the host bone); the HA collar promotes direct bone ingrowth and ongrowth at the host bone-prosthesis interface, reducing the stress concentration at the bone-stem junction and decreasing aseptic loosening rates; the Stanmore SMILES system (Stanmore Modular Individualised Lower Extremity System) uses a titanium alloy stem with an HA-coated collar; Coathup et al. demonstrated significantly lower loosening rates with HA-collared vs non-collared distal femoral mega-prostheses
- Silver coating for infection prophylaxis: silver-coated mega-prostheses (MUTARS — Modular Universal Tumour And Revision System; Implantcast) have a silver-ion-releasing surface that provides antimicrobial protection; silver ions disrupt bacterial cell membranes and inhibit biofilm formation; silver-coated prostheses significantly reduce early deep infection rates compared to uncoated titanium (approximately 50% reduction in early infection in the first 6 months post-implantation); the silver coating is gradually worn off over time, reducing its protective effect for late infections; silver-coated prostheses are approximately 5–7% more expensive; no significant systemic silver ion toxicity reported in published series
- Key systems: Stanmore SMILES (RNOH, UK); MUTARS (Implantcast, Germany); GMRS (Global Modular Replacement System — Stryker); LPS (Limb Preservation System — DePuy); MRS (Modular Replacement System — Biomet/Zimmer)
Site-Specific Considerations
| Site | Key Features | Critical Reconstructive Step |
|---|---|---|
| Distal femur (most common) | Rotating hinge knee mechanism (rotating hinge allows axial rotation — reduces rotational torque on the stem-bone interface vs fixed hinge); Myers et al. 10-year data: 50% reduction in aseptic loosening with rotating vs fixed hinge design; stem — intramedullary into femoral diaphysis; MSTS scores 80–87% for osteosarcoma distal femur series (246 cases — Natarajan et al.) | Extensor mechanism reconstruction: the quadriceps tendon / patellar tendon must be reattached to the prosthesis; medial gastrocnemius flap — the most reliable method (rotates to cover the prosthesis and augment the extensor mechanism); direct tendon-to-prosthesis suturing through anterior holes; poor extensor mechanism = extension lag + functional impairment |
| Proximal tibia | Highest soft tissue complication rate of any mega-prosthetic site — the proximal tibia has very little soft tissue coverage; patellar tendon attachment to tibial tubercle is lost in resection | Mandatory gastrocnemius flap for coverage (medial or lateral); patellar tendon reattachment through prosthesis anteriorly; without flap → wound breakdown and deep infection |
| Proximal femur | Proximal femoral replacement or hemiarthroplasty; the abductor mechanism (gluteus medius insertion to greater trochanter) is typically disrupted or sacrificed at resection | Abductor reconstruction: the remaining gluteus medius and minimus must be reattached to the prosthesis through drill holes or dedicated attachment points; without abductor repair → Trendelenburg gait + hip instability; dual mobility acetabular cup used to reduce dislocation risk (large effective head size) |
| Proximal humerus | Proximal humeral replacement; rotator cuff typically sacrificed in resection; glenohumeral instability a major functional concern | Rotator cuff remnants and deltoid must be reattached through prosthesis holes; MSTS scores typically 60–80%; shoulder function remains limited (no rotator cuff) but pain relief is good; patients often prefer shoulder prosthesis over amputation despite functional limitation |
| Total femur replacement (TFR) | The entire femur is replaced with a mega-prosthesis articulating with the acetabulum proximally (bipolar cup or total hip) and the tibia distally (rotating hinge knee); indications — massive femoral tumour involving the entire femur; combined proximal and distal femur periprosthetic infection with a small intact diaphyseal segment; failed hip and knee arthroplasty with stems nearly touching; at least 12 cm of remaining bone needed for standard stem fixation — if <12 cm, total femur replacement considered | All soft tissue attachments (quadriceps, adductors, glutei) must be reattached to the prosthesis; MSTS score 66% average; 2–14 year overall survival 82% (Jaiswal et al.) |
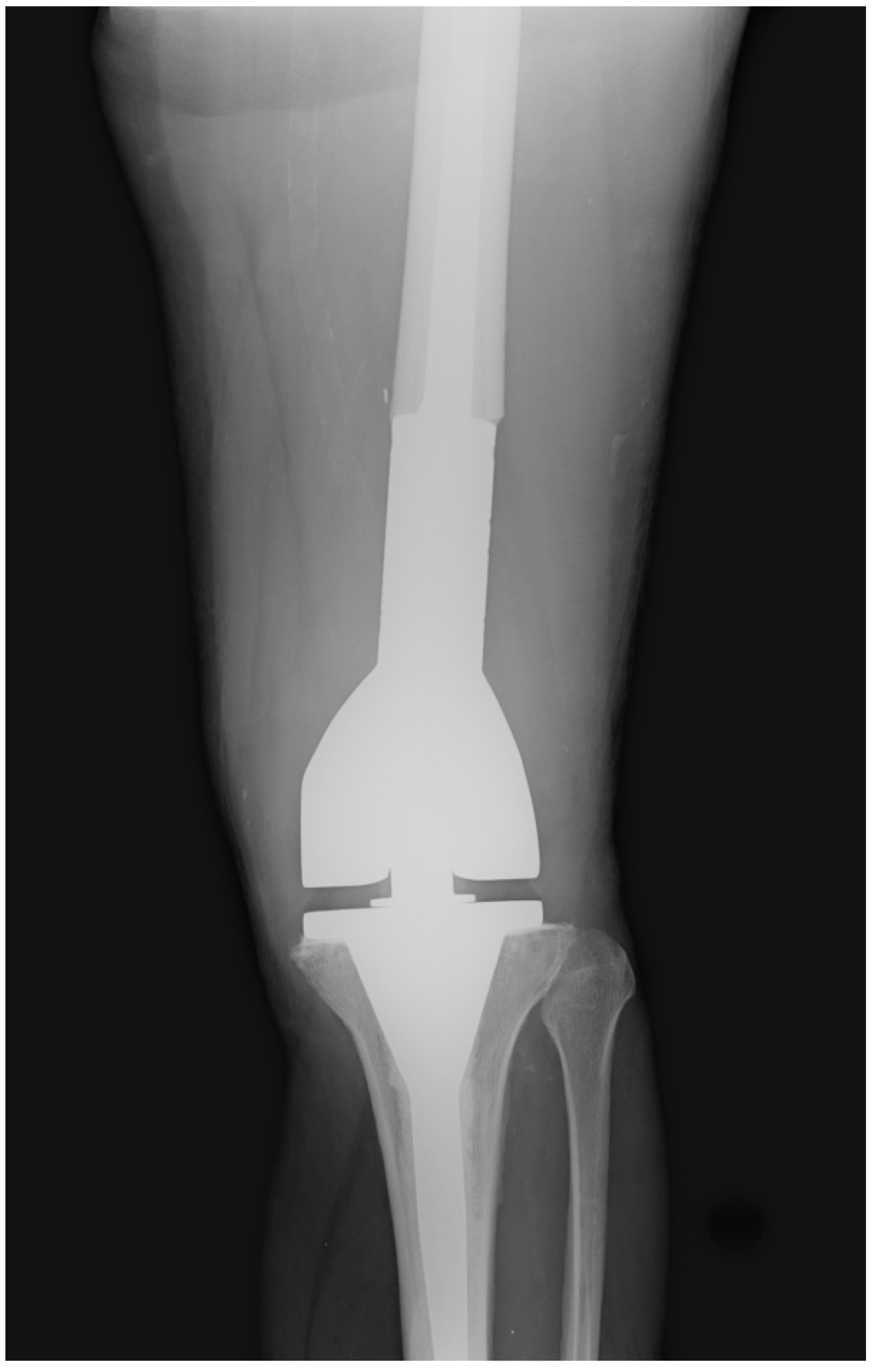
Complications — Henderson Classification
- Henderson Type I — Soft tissue failure (12% of all failures; absolute incidence 2.9% — Henderson et al. multicentre series): disruption or incompetence of periarticular soft tissue attachments (ligaments, tendons) leading to instability or extensor mechanism failure; most common around the shoulder and hip (where soft tissue is critical for stability); proximal tibia resection has highest soft tissue failure rate; prevention — meticulous soft tissue reconstruction at primary surgery (gastrocnemius flap for proximal tibia; rotator cuff reattachment for proximal humerus; abductor reattachment for proximal femur)
- Henderson Type II — Aseptic loosening: incidence 4.9–9.9% at the distal femur (Unwin et al. — 1001 Stanmore prostheses: 9.9% loosening at distal femur, 6.5% proximal tibia, 2.3% proximal femur); lower loosening rates with HA-coated collars and rotating hinge design; stem loosening is managed by revision to a longer/larger stem; cement versus cementless stem fixation: cemented stems provide immediate stability (preferred in elderly non-oncological patients); cementless press-fit with HA collar preferred in oncological patients (avoiding cement mantle complications; theoretical advantage for revision if required)
- Henderson Type III — Structural failure (0–7.7%): mechanical failure of the prosthesis — stem fracture, hinge failure, modular junction fatigue; most common at the rotating hinge knee joint; modern materials (titanium alloy stem; cobalt-chrome hinge; UHMWPE bushing) have reduced this significantly; bushing wear at the rotating hinge requires periodic bushing exchange (analogous to PE bushing exchange in semi-constrained TEA)
- Henderson Type IV — Infection: the most common complication across all mega-prosthetic sites; reported in 5–15% of cases; risk is higher in proximal tibial resections (thin soft tissue envelope), immunocompromised patients (on chemotherapy), and revision non-oncological cases; management — debridement and implant retention (DAIR) has low success in mega-prosthetic infection; two-stage revision (antibiotic cement spacer + reimplantation) is the standard; silver-coated prostheses (MUTARS) reduce early infection rates; amputation may be required for uncontrolled infection in oncological patients if margins are adequate
- Henderson Type V — Tumour progression: local recurrence or distant metastasis requiring change in surgical management; the most important outcome determinant in paediatric and young adult oncological patients; adequate oncological margins at resection are non-negotiable — functional outcome is secondary to oncological clearance; local recurrence after mega-prosthetic limb salvage typically requires amputation
Consultant-Level Considerations
- Mirels scoring system for metastatic bone disease: guides prophylactic fixation decisions for impending pathological fractures; scores site (upper limb/lower limb/pertrochanteric), pain (mild/moderate/severe), lesion type (blastic/mixed/lytic), and cortical destruction (<1/3, 1/3–2/3, >2/3); score 0–12; score ≥9 = high risk of fracture → prophylactic fixation or mega-prosthesis; score ≤7 = low risk → radiation therapy; score 8 = borderline; for metastatic distal femoral lesions not amenable to intramedullary nail or plate fixation (e.g., destruction of the condyles), a distal femoral replacement mega-prosthesis provides immediate stability and pain relief
- The rotating hinge vs fixed hinge debate: the shift from fixed to rotating hinge knee mega-prostheses was one of the most clinically significant implant evolution steps; the rotating hinge allows axial tibio-femoral rotation (the natural internal rotation of the tibia in flexion), reducing rotational torque transfer to the stem; Myers et al. demonstrated a greater than 50% reduction in aseptic loosening rates at 10 years with rotating versus fixed hinge in proximal tibial and distal femoral replacements; all modern mega-prosthetic knee designs use rotating hinges
- Functional outcome scoring — MSTS score: the Musculoskeletal Tumour Society (MSTS) score is the standard functional outcome tool in orthopaedic oncology; scores pain, function, and emotional acceptance on a scale of 0–5 for each; maximum 30 points (expressed as percentage); MSTS >70% = good; >85% = excellent; average MSTS scores for distal femur mega-prosthesis in published series: 80–87%; proximal humerus: 60–75%; total femur: 65–70%; outcomes are better in younger patients who adapt better to altered biomechanics
Exam Pearls
- Mega-prosthesis indications: primary malignant bone tumour (osteosarcoma, Ewing, chondrosarcoma); metastatic disease with impending fracture (Mirels ≥9); failed arthroplasty with massive bone loss (AORI III, Paprosky IIIB); complex periprosthetic fractures; distal femur non-union in elderly
- Modular design advantage: intraoperative adjustment to exact resection length; avoids pre-manufacturing mismatch of custom monoblock designs; allows future modular component exchange
- HA collar: hydroxyapatite-coated ring at bone-prosthesis junction; promotes bone ongrowth/ingrowth; reduces aseptic loosening; standard feature of modern Stanmore SMILES and similar systems
- Silver coating (MUTARS): antimicrobial ion release; ~50% reduction in early infection rates; gradually wears off — protective mainly for first 6 months; 5–7% more expensive; no significant systemic toxicity
- Rotating hinge knee: allows axial rotation → reduces rotational torque on stem; Myers et al. — >50% reduction in 10-year aseptic loosening vs fixed hinge; standard in all modern knee mega-prostheses
- Henderson classification: Type I (soft tissue — most common at shoulder/hip; highest at proximal tibia); Type II (aseptic loosening — 4.9–9.9%; reduced by HA collar + rotating hinge); Type III (structural failure — stem fracture, hinge failure, bushing wear); Type IV (infection — 5–15%; silver coating ± two-stage revision); Type V (tumour progression — indicates amputation if uncontrollable)
- Proximal tibia reconstruction: HIGHEST soft tissue complication rate; mandatory medial gastrocnemius flap for coverage + extensor mechanism attachment; without flap → wound dehiscence → deep infection
- Total femur replacement: entire femur replaced; indications — massive femoral tumour; combined hip + knee PJI with <12 cm intact diaphysis; failed THA + TKA with stems nearly touching; MSTS ~66%; bipolar or THA proximally + rotating hinge distally
- MSTS score: standard oncological outcome tool; max 30 (100%); >70% = good; >85% = excellent; distal femur 80–87%; proximal humerus 60–75%; total femur 65–70%
- Mirels score ≥9: prophylactic fixation or mega-prosthesis for impending pathological fracture; lytic >2/3 cortex + lower limb + severe pain = maximum risk
